Literature Review on Polypharmacy Related Falls in the Elderly
- Research article
- Open Access
- Published:
Polypharmacy is a take a chance factor for hospital admission due to a fall: bear witness from the English language Longitudinal Study of Ageing
BMC Public Wellness volume xx, Article number:1804 (2020) Cite this article
Abstract
Background
Falls among older people are common; however, around 40% of falls could exist preventable. Medications are known to increase the risk of falls in older adults. The debate nearly reducing the number of prescribed medications remains controversial, and more evidence is needed to sympathise the relationship betwixt polypharmacy and fall-related hospital admissions. Nosotros examined the result of polypharmacy on hospitalization due to a autumn, using a large nationally representative sample of older adults.
Methods
Data from the English Longitudinal Study of Ageing (ELSA) were used. We included 6220 participants aged 50+ with valid information nerveless between 2012 and 2018.The principal result measure was hospital access due to a autumn. Polypharmacy -the number of long-term prescription drugs- was the main exposure coded every bit: no medications, 1–4 medications, 5–9 medications (polypharmacy) and 10+ medications (heightened polypharmacy). Competing-risk regression analysis was used (with death equally a potential competing risk), adjusted for common confounders, including multi-morbidity and fall risk-increasing drugs.
Results
The prevalence of people admitted to infirmary due to a fall increased according to the number of medications taken, from 1.5% of falls for people reporting no medications, to 4.7% of falls among those taking 1–4 medications, 7.9% of falls among those with polypharmacy and fourteen.8% among those reporting heightened polypharmacy. Fully adjusted SHRs for hospitalization due to a fall amid people who reported taking ane–4 medications, polypharmacy and heightened polypharmacy were 1.79 (one.eighteen; ii.71), 1.75 (1.04; two.95), and 3.19 (1.61; half dozen.32) respectively, compared with people who were not taking medications.
Conclusions
The risk of hospitalization due to a fall increased with polypharmacy. Information technology is suggested that prescriptions in older people should be revised on a regular basis, and that the number of medications prescribed be kept to a minimum, in order to reduce the adventure of fall-related hospital admissions.
Groundwork
Falls, defined as an unanticipated incident in which a person come to rest on the ground or a lower level, [ane] are the nigh frequent type of accidents amongst older people [2]. One in three people over 65 years of age experience at least one autumn each year, and injuries occur in approximately 20% of such cases [3]. Older people who accept suffered a fall experience an increased hazard of recurrence and of being hospitalized. Falls not only carry a homo brunt, but they tin incur considerable medical care costs, with estimates beingness suggested betwixt 0.85 and 1.5% of total healthcare expenditure in the Britain [4].
Information technology has been estimated that around 40% of falls in older people are preventable [5]. Equally a outcome, a big torso of inquiry has emerged to explore risk factors that might decide whether someone is at risk of experiencing a fall, especially a fall for which they might require treatment in hospital. Polypharmacy, defined as the chronic co-prescription of multiple medications, has been identified every bit one of the most significant factors associated with falls among older people [six, 7]. Several studies in ageing populations have reported that the adventure of a fall increases with the use of four or more than medications [8,nine,10,11,12,13,14,fifteen,xvi]. Notwithstanding, older adults using multiple medications might also have several long-term weather, whose pharmacological treatment often requires the concomitant use of several medications. Therefore, the chance of falls might not exist contained of these long-term weather condition. Indeed, those with multimorbidity (defined equally reporting iii or more than long-term weather condition) who also take multiple medications have a higher chance of falls [17].
Contempo studies also propose that medications such equally cardiovascular agents, central nervous organization drugs, analgesics and endocrine drugs, increase the adventure of falls [14, 15]. The possible underlying mechanisms for the increased risk of falls related to the use of these medications, called "fall run a risk-increasing drugs" (FRIDs), relate to the adverse effects (eg, dizziness, imbalance or mobility difficulties, reduced attention and vigilance). However, Seppala et al., in their systematic review, bespeak out that adjustment for long-term conditions and "fall risk-increasing drugs" has rarely been carried out in studies of polypharmacy and falls [18]. Properly adjusting for both is imperative, since polypharmacy is often the event of long term conditions, [19] and the risk of polypharmacy on falls may non be contained of "fall risk-increasing drugs" [14].
The argue about reducing the number of prescribed medications remains controversial. On the one manus, the prescription of several medications is largely justified by the complex clinical profile of older adults and information technology has been shown that interventions to reduce the number of concurrent medications have been unsuccessful [xx,21,22]. On the other hand, studies have shown that medication withdrawal, especially FRIDs, has been constructive in reducing the risk of falls [23]. Therefore, more evidence is needed to understand the relationship between polypharmacy and fall-related hospital admissions. Big nationally representative longitudinal studies of ageing, which collect a broad range of factors and have been linked to administrative wellness information, are best placed to provide insights into this relationship. Accordingly, the aim of this study is to examine, in a nationally representative sample of older adults, whether polypharmacy is a risk gene for hospitalization due to a fall. We will examine this independently of other risk factors, including long-term conditions and drugs known to increment the run a risk of falling (FRIDs).
Methods
Information
These data are from the English Longitudinal Study of Ageing (ELSA) [24] a nationally representative sample of individuals anile fifty and older living in individual households in England, followed and re-interviewed every 2 years. The master objective of the study is to understand the complex dynamics of the ageing process, that is the relationships betwixt economic and family circumstances, behaviour, social participation, biological science, retirement, and health and well-being. The written report began in 2002–2003 (starting time phase of data drove referred to as moving ridge i). Data collection comprises face up-to-face interviews, self-completion questionnaires and nurse visits in participants' homes every other moving ridge. For the purpose of this written report, we used data from wave 6 (2012–2013) as our baseline, when information on medication was first collected during the nurse visit. A total of 6220 individuals had valid data on medications and covariates of interest at baseline. All individuals included in the baseline sample (2012–2013) had their information linked to Infirmary Episode Statistics, and to mortality even those who dropped out of the report later on baseline.
Outcome measure
Hospitalization due to a autumn was derived from the Infirmary Episode Statistics data linked by NHS digital to ELSA participants' NHS number, date of birth, gender and postcode. All participants were followed-up from the interview date up to March 2018. For each participant, a record of each hospitalization to secondary care is available, with admission date, episode elapsing, principal diagnosis and secondary diagnoses. Diagnoses are coded according to the international classification of illness tenth version (ICD-10). Falls correspond to the ICD-10 codes W00 to W19. The event "fall" is defined as the beginning episode where a chief diagnosis of fall was recorded.
Exposure: polypharmacy
At wave six (2012–2013) during the nurse visits to participants' homes nurses recorded medications taken by each participant. These drugs, both generic and brand name, were allocated codes based on the British National Formulary. In the definition of polypharmacy, only long-term medications were considered. Long-term medications were either drugs for long-term diseases such every bit diabetes and hypertension, or drugs for long-term symptoms such as sedatives. Despite variation, which exists in the definition of polypharmacy, the number of medications in this sample was recoded according to the most normally used cut-offs: No medications, one–four medications, five–9 medications (polypharmacy) and x or more medications (heightened polypharmacy) [25].
Potential confounders
Socio-demographic variables included age (continuous, ranging from 54 to 101 at moving ridge half-dozen), sexual activity (males vs females), cohabitation status (currently living or not with a partner whether married or not), and educational attainment (high-college and higher up, medium-A-levels, low-beneath O-levels). For cerebral function we used a memory score computed from a discussion-list learning examination [26] in which a list of x words was read out to report participants, who were then asked to remember as many words as possible immediately and afterward around a five-minute delay (full score ranged from 0 to 20 with higher scores indicating better cerebral function). Health behaviours included frequency of alcohol intake (in days) in the final 12 months ascertained from self-reported responses and coded as daily (5/7 days week) or less than daily (< v days a calendar week); smoking condition (non-smoker vs electric current smoker); body mass index (computed from objectively measured elevation and weight); physical activity (agile vs sedentary). Physical activity was measured using responses to questions on leisure-fourth dimension physical activity and aggregated to compute a five-level score from inactive to active, and used in the assay as binary. We as well used a self-reported measure of eyesight (poor vs good). Health conditions were ascertained from self-reported md diagnosis and included: coronary heart disease (CHD), stroke, diabetes, depression (defined as 4 or more than depressive symptoms), respiratory illness, arthritis, cancer, dementia, Parkinson's illness and Alzheimer'southward disease. In addition we computed a variable for multimorbidity past recoding the number of long-term weather condition reported into a dichotomous variable, with a cut-off of iii or more than [16]. FRIDs were also taken into account as a binary variable (2+ FRIDS versus none). FRIDs included cardiovascular agents, cardinal nervous system drugs (not including antiparkinsonians), analgesics (non-steroidal anti-inflammatory drugs), thyroid drugs, and antihyperglycemic drugs [14]. Physical functioning was measured using number of limitations with mobility items (continuous) and the number of difficulties with activities of daily living (ADLs) and instrumental activities of daily living (IADLs) (binary, one or more versus no difficulties), and cognitive part. ADLs items were: dressing, walking across a room, bathing or showering, eating, getting out of bed, using the toilet; IADLs items were: using a map, preparing a hot meal, shopping for groceries, making phone calls, taking medications, doing piece of work around the house, managing money.
Statistical analysis
To examine the association betwixt polypharmacy and hospitalization due to a fall nosotros employed competing-hazard regression analysis with subdistribution adventure ratios (SHR) and related 95% Confidence Intervals, using a version of the Fine and Gray method [27]. This method allows a competing hazard – an event that might occur during the follow-up instead of the event of interest – to be taken into account in the assay. In this example, decease is a potential competing take a chance when examining incidence rates of admission to infirmary due to a autumn; therefore, it is important to take this into account, rather than treating those who had died as censored. Mortality status was ascertained from linked register data, up to the terminate of March 2018. By the cease of this follow-upwardly menses (six years) 295 admissions to hospital due to a autumn were recorded and 594 deaths occurred.
In a sensitivity analysis, we explored whether autumn hospitalization was associated with the utilize of polypharmacy also amid people in the 0–one FRID category, as previous studies suggested that the adventure of polypharmacy of falls might not be associated with fall risk, independently of FRIDs [9, 14].
Results
The baseline characteristics of the sample in 2012–2013 according to polypharmacy status are reported in Table 1. The prevalence of people admitted to hospital due to a fall increased steadily according to polypharmacy status. This ranged from 1.5% in people reporting no medications, to iv.vii% of falls among people reporting 1–4 medications, 7.9% of falls occurred amongst people with polypharmacy (5–ix medications) and 14.8% amid those reporting heightened polypharmacy (10 + medications). Respondents reporting polypharmacy and heightened polypharmacy were besides older and reported poorer health outcomes at baseline than those not taking medications.
The unadjusted cumulative incidence function shows a dose-response association in the risk of hospitalization due to a fall and polypharmacy; in detail, the cumulative incidence curve for ten+ medications increased steeply with time (Fig. 1).
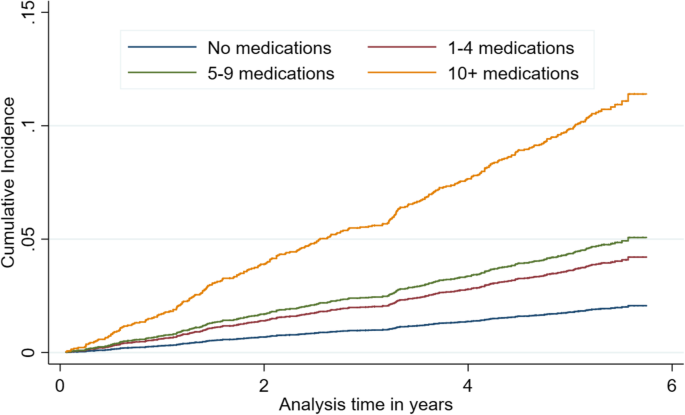
Estimates of the cumulative incidence curves of hazard of hospitalization following a fall according to polypharmacy, England 2012–2018
In Tabular array ii we study the subdistribution risk ratios (SHR) for the association between polypharmacy and risk of hospitalization due to a fall estimated using competing risk analysis. The age- and sex- adjusted SHRs for hospitalization due to a autumn amidst people who reported taking 1–4 medications, polypharmacy and heightened polypharmacy were 2.06 (95%CI:one.38;3.07), 2.49 (95%CI:1.62;3.82), and v.79 (95%CI:iii.33;ten.one) respectively, compared with people who were not taking medications. After adjustment for all covariates, the association betwixt polypharmacy and hospitalization due to a fall, reduced to ane.79 (95%CI:1.18; ii.71) among people who reported taking 1–4 medications, reduced to i.75 (95%CI: one.04; 2.95) amongst those reporting polypharmacy and was 3.19 (95%CI: 1.61; vi.32) for heightened polypharmacy.
In farther sensitivity analysis, we investigated whether the association between polypharmacy and admissions to infirmary due to a fall remained when FRIDs were included in the model. We ran the analyses again amid those who were taking 0–1 FRIDs. We found that the clan betwixt polypharmacy and hospitalization due to a fall reduced in magnitude, but was still statistically meaning by polypharmacy condition, including the group of one–4 medications (SHR 1.65 95%1.one;ii.v p = 0.025 compared to not taking medications).
Discussion
Using a large nationally representative sample of older people in England, our written report showed a strong association betwixt polypharmacy status and the gamble of hospitalization due to a fall. Nosotros found that the adventure was highest amid people reporting polypharmacy and heightened polypharmacy compared to those who reported taking no medications. We also observed a slightly elevated risk amidst older adults who reported the concurrent use of i–four medications compared with those who reported taking none. These associations were not explained by mutual risk factors for falls, neither past multi-morbidities nor past FRIDs.
In agreement with results from a population-based instance control study of people 65 years and older living in Stockholm, [12] we found that the use of one or more medications led to an increased take a chance of hospitalization due to a autumn. In a previous investigation using data from ELSA [viii] it was plant that polypharmacy and heightened polypharmacy significantly increased the gamble of falls among people aged 60 and over, withal, the study but used a short follow-up menstruation (two years) and a self-reported measure of falls. Our analysis has improved the results of previous studies by using an objective measure of falls and by studying a younger cohort at the first assessment (anile 50 years quondam and over) [8, 9, eleven,12,xiii,14]. Furthermore, we showed that this increased risk of falls amid people taking medications was contained of long-term conditions and FRIDs.
Falls are common among older adults, and as the proportion of elderly people in the population continues to increase, falls in this group are predicted to pose a serious brunt on healthcare expenditure. Strategies to prevent falls include the identification of potential modifiable risk factors, such as multiple medications [6]. Our results contribute to current discussions in the U.k. nearly reducing the number of prescribed medications in older age. The National Institute for Health and Care Excellence published new guidelines for the direction of multimorbidity amidst individuals taking 10 or more prescribed medications. Nonetheless, we take shown that the risk of hospitalization due to a fall is also loftier in patients taking 1–four and 5–9 medications, and these people might be excluded from the target group for medication reviews [28]. Period reviews of prescriptions among older patients should be in identify to assure that the number of medications consumed is minimalized, particularly amongst frail people who might be at higher risk of falling.
Strengths and limitations
This written report examined the association between polypharmacy and hospitalization due to a fall in a nationally representative sample of not-institutionalised individuals in England. The utilise of medication data nerveless by a nurse, and hospital administrative data, is less susceptible to recall bias. Moreover, we considered the number of long-term conditions from which participants suffered and were able to conform for these in our analyses. Lastly, nosotros used a competing risk analysis strategy to consider mortality as a competing consequence.
The main limitation of our study is that the data on medication was collected for the first time in 2012/2013; it would have been preferable to accept multiple fourth dimension points of medication records to establish whether the elapsing of polypharmacy had an impact on the risk of beingness admitted to hospital due to a fall. We were able to investigate the number of medications prescribed, simply unfortunately, we were non able to explore the nature of these medications, since the specific drug name was ofttimes not bachelor. Nosotros were also not able to test common drug-drug interactions directly, [29] such every bit with antihypertensive, diuretics and selective serotonin reuptake inhibitors (SSRIs) [30]. Potentially serious drug-drug interactions take been reported in drugs recommended past clinical guidelines for different long-term conditions, such as cardiovascular diseases, type two diabetes, depression and dementia [29, 31]. Astringent drug-drug interactions could happen between SSRIs and serotonin–norepinephrine reuptake inhibitors or betwixt beta-blockers and certain antiarrhythmic agents; we cannot entirely exclude that these interactions occurred in our sample [29, 31]. Future studies should examine specific drug-drug interactions in detail [31].
An additional issue is that the cess of polypharmacy was based on the long-term medications that were being taken by participants at the time of the nurse visits. Although excluded medications were primarily painkillers, a small proportion of antihistamines, both sedating and not-sedating types, were likewise excluded. Furthermore, we do not have information nigh whether the medication prescribed changed over the follow-upward catamenia. People might too accept taken other medications acutely that might have provoked problems with remainder and increased risk of falls.
It is also possible that the risk of falls may be increased by strong doses of FRIDs, merely nosotros did not have data on medication dosage. Finally, although nosotros used a broad range of confounders, some balance confounding might exist. For instance, nosotros could not adjust for objective measures of physical functioning since those were collected simply amongst those aged 60 and over.
Conclusions
In conclusion, we found that the risk of hospitalization due to a fall increased with polypharmacy status. The increased run a risk was apparent amidst those reporting polypharmacy and heightened polypharmacy, just also among those reporting the concurrent employ of 1–iv medications. Information technology is advisable that drug prescriptions in older people be revised on a regular basis, and that the number of medications should exist kept to the minimum possible as information technology might reduce the risk of fall-related hospital admissions.
Availability of data and materials
The ELSA datasets are available in the UK Information Service, [https://beta.ukdataservice.ac.britain/datacatalogue/series/series?id=200011].
Hospital Episode Statistics data and mortality information will be made available in due course.
Abbreviations
- ADLs:
-
Activities of Daily Living
- CHD:
-
Coronary Center Disease
- ELSA:
-
English Longitudinal Study of Ageing
- FRIDs:
-
Autumn Risk-Increasing Drugs
- IADLs:
-
Instrumental Activities of Daily Living
- ICD-10:
-
International Classification of Disease
- SHR:
-
Subdistribution Run a risk Ratios
References
-
Lamb SE, Jorstad-Stein EC, Hauer K, Becker C. Prevention of falls network East, outcomes consensus G. development of a common upshot information set for fall injury prevention trials: the prevention of falls network Europe consensus. J Am Geriatr Soc. 2005;53(9):1618–22.
-
Gale CR, Cooper C, Aihie SA. Prevalence and chance factors for falls in older men and women: the English longitudinal study of ageing. Age Ageing. 2016;45(6):789–94.
-
Lord S, Sherrington C, Menz H. Falls in older people. Chance factors and strategies for prevention. Cambridge: University Press; 2001.
-
Heinrich A, de la Rosa S, Schneider BA. The part of stimulus complication, spectral overlap, and pitch for gap-detection thresholds in young and old listeners. J Acoust Soc Am. 2014;136(4):1797–807.
-
Tinetti ME, Speechley Thou. Prevention of falls among the elderly. N Engl J Med. 1989;320(16):1055–nine.
-
Zia A, Kamaruzzaman SB, Tan MP. Polypharmacy and falls in older people: balancing testify-based medicine against falls risk. Postgrad Med. 2015;127(3):330–vii.
-
Burt J, Elmore N, Campbell SM, Rodgers Southward, Avery AJ, Payne RA. Developing a mensurate of polypharmacy appropriateness in primary care: systematic review and adept consensus study. BMC Med. 2018;16(one):91.
-
Dhalwani NN, Fahami R, Sathanapally H, Seidu S, Davies MJ, Khunti 1000. Association between polypharmacy and falls in older adults: a longitudinal report from England. BMJ Open. 2017;vii(10):e016358.
-
Ziere G, Dieleman JP, Hofman A, Pols HA, van der Cammen TJ, Stricker BH. Polypharmacy and falls in the middle age and elderly population. Br J Clin Pharmacol. 2006;61(two):218–23.
-
Wong H, Heuberger R, Logomarsino J, Hewlings Southward. Associations between alcohol utilise, polypharmacy and falls in older adults. Nurs Older People. 2016;28(i):30–half-dozen.
-
Baranzini F, Diurni M, Ceccon F, Poloni N, Cazzamalli Southward, Costantini C, et al. Fall-related injuries in a nursing abode setting: is polypharmacy a risk factor? BMC Wellness Serv Res. 2009;ix:228.
-
Helgadottir B, Laflamme L, Monarrez-Espino J, Moller J. Medication and autumn injury in the elderly population; practice individual demographics, health status and lifestyle matter? BMC Geriatr. 2014;xiv:92.
-
Kojima T, Akishita M, Nakamura T, Nomura K, Ogawa S, Iijima K, et al. Polypharmacy as a adventure for fall occurrence in geriatric outpatients. Geriatr Gerontol Int. 2012;12(iii):425–30.
-
Zia A, Kamaruzzaman SB, Tan MP. The consumption of 2 or more fall gamble-increasing drugs rather than polypharmacy is associated with falls. Geriatr Gerontol Int. 2017;17(3):463–70.
-
Richardson K, Bennett K, Kenny RA. Polypharmacy including falls risk-increasing medications and subsequent falls in community-dwelling eye-aged and older adults. Age Ageing. 2015;44(1):ninety–6.
-
Morin Fifty, Calderon Larranaga A, Welmer AK, Rizzuto D, Wastesson JW, Johnell Thou. Polypharmacy and injurious falls in older adults: a nationwide nested instance-control study. Clin Epidemiol. 2019;11:483–93.
-
Damian J, Pastor-Barriuso R, Valderrama-Gama East, de Pedro-Cuesta J. Factors associated with falls among older adults living in institutions. BMC Geriatr. 2013;thirteen:vi.
-
Seppala LJ, van de Glind EMM, Daams JG, Ploegmakers KJ, de Vries M, Wermelink A, et al. Fall-Hazard-Increasing Drugs: A Systematic Review and Meta-analysis: III. Others. J Am Med Dir Assoc. 2018;19(iv):372 e1–viii.
-
Morin 50, Johnell G, Laroche ML, Fastbom J, Wastesson JW. The epidemiology of polypharmacy in older adults: register-based prospective cohort study. Clin Epidemiol. 2018;10:289–98.
-
Salisbury C, Human MS, Bower P, Guthrie B, Chaplin 1000, Gaunt DM, et al. Management of multimorbidity using a patient-centred intendance model: a pragmatic cluster-randomised trial of the 3D arroyo. Lancet. 2018;392(10141):41–50.
-
Wallace E, Salisbury C, Guthrie B, Lewis C, Fahey T, Smith SM. Managing patients with multimorbidity in chief intendance. BMJ. 2015;350:h176.
-
Wise J. Polypharmacy: a necessary evil. BMJ. 2013;347:f7033.
-
Gillespie LD, Robertson MC, Gillespie WJ, Sherrington C, Gates Southward, Clemson LM, et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2012;nine:CD007146.
-
Steptoe A, Breeze E, Banks J, Nazroo J. Cohort contour: the English longitudinal written report of ageing. Int J Epidemiol. 2013;42(six):1640–8.
-
Masnoon North, Shakib Southward, Kalisch-Ellett 50, Caughey GE. What is polypharmacy? A systematic review of definitions. BMC Geriatr. 2017;17(one):230.
-
Zaninotto P, Batty GD, Allerhand Yard, Deary IJ. Cognitive function trajectories and their determinants in older people: eight years of follow-up in the English longitudinal study of ageing. J Epidemiol Community Wellness. 2018;72(8):685–94.
-
Fine JP, Grey RJ. A proportional hazards model for the subdistribution of a competing adventure. J Am Stat Assoc. 1999;94:496–509.
-
Farmer C, Fenu East, O'Flynn Due north, Guthrie B. Clinical assessment and management of multimorbidity: summary of Dainty guidance. BMJ. 2016;354:i4843.
-
Dumbreck South, Flynn A, Nairn M, Wilson M, Treweek S, Mercer SW, et al. Drug-disease and drug-drug interactions: systematic examination of recommendations in 12 UK national clinical guidelines. BMJ. 2015;350:h949.
-
Andersson ML, Bottiger Y, Kockum H, Eiermann B. High prevalence of drug-drug interactions in master wellness intendance is caused by prescriptions from other healthcare units. Basic Clin Pharmacol Toxicol. 2018;122(5):512–6.
-
Strandell J, Caster O, Hopstadius J, Edwards IR, Noren GN. The evolution and evaluation of triage algorithms for early discovery of adverse drug interactions. Drug Saf. 2013;36(v):371–88.
Acknowledgements
Not applicative.
Funding
The English Longitudinal Study of Ageing is supported by the National Institute on Crumbling (grant numbers: 2RO1AG7644 and 2RO1AG017644-01A1) and a consortium of the UK government departments coordinated past the National Constitute for Health Research. The funding bodies had no part in the study design; in the drove, analysis, and interpretation of data; in the writing of the manuscript; and in the decision to submit the manuscript for publication.
Author data
Affiliations
Contributions
All authors contributed to the written report concept and blueprint. PZ wrote the first and successive drafts of the paper. YTH prepared the polypharmacy data. CL and JA prepared the HES data. PZ carried out all the statistical analysis with assist from GDG. All authors contributed to the interpretation of results and approved the final version of the paper.
Corresponding writer
Ideals declarations
Ethics approval and consent to participate
The ELSA report was conducted in accordance with the Declaration of Helsinki and ethical approving and experimental protocols were granted by NHS Research Ethics Committees under the National Enquiry and Ethics Service.
Participants provided informed written consent to the investigation.
Consent for publication
Non applicable.
Competing interests
The author(s) declare that they take no competing interests.
Boosted information
Publisher'southward Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed nether a Artistic Commons Attribution iv.0 International License, which permits apply, sharing, adaptation, distribution and reproduction in whatever medium or format, as long every bit you give advisable credit to the original author(southward) and the source, provide a link to the Creative Commons licence, and bespeak if changes were made. The images or other third party textile in this commodity are included in the article's Creative Eatables licence, unless indicated otherwise in a credit line to the fabric. If textile is not included in the article's Artistic Commons licence and your intended use is non permitted by statutory regulation or exceeds the permitted employ, you will need to obtain permission directly from the copyright holder. To view a re-create of this licence, visit http://creativecommons.org/licenses/by/iv.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made bachelor in this article, unless otherwise stated in a credit line to the data.
Reprints and Permissions
About this article
Cite this commodity
Zaninotto, P., Huang, Y.T., Di Gessa, Thou. et al. Polypharmacy is a risk factor for infirmary admission due to a fall: evidence from the English language Longitudinal Study of Ageing. BMC Public Health 20, 1804 (2020). https://doi.org/10.1186/s12889-020-09920-10
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s12889-020-09920-x
Keywords
- Older people
- Polypharmacy
- Falls
- Hospitalization
mikesellwitheitay.blogspot.com
Source: https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-020-09920-x
0 Response to "Literature Review on Polypharmacy Related Falls in the Elderly"
Postar um comentário